This web page was produced as an assignment for Genetics 564, an undergraduate course at UW-Madison.
The Disease: Schizophrenia
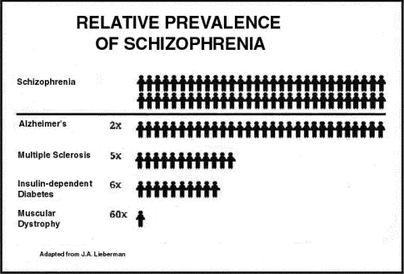 An image of the relative prevalence of Schizophrenia in the general public.
An image of the relative prevalence of Schizophrenia in the general public.
Schizophrenia is a severe, chronic brain disorder that causes one to interpret reality abnormally [1,2]. The word 'schizophrenia' comes from the Greek word 'skhizein,' which means 'to split' and the Greek word 'phrenos,' which means 'diaphragm, heart, mind' [3]. However, schizophrenia is not a split personality disorder, the split in the term's Greek origins refers to the disruption in the usual balance in emotions and thinking [1].
Schizophrenia affects men and women equally and occurs at similar rates in all ethnicities world wide. However, an australian study found that schizophrenia is more common in developed countries and more common in women in developing countries [6]. In fact, schizophrenia ranks among the top ten causes of disability in developed countries worldwide [5]. Roughly 1% of Americans have schizophrenia [2]. Worldwide, roughly 0.7-1.2% of adults have schizophrenia at some point in their lives [3]. Schizophrenia is known to run in families; it occurs in 10% of people with a direct relative, such as a parent or sibling, who have the disease. An identical twin of a schizophrenic has a 40-65% chance of developing schizophrenia [2]. However, schizophrenia is a complex disease, meaning that there are several genes associated with an increased risk for the disease. There is not a single gene that causes schizophrenia [2]. These genes are generally involved in brain development and the formation of important brain chemicals [2]. The exact cause(s) of schizophrenia are not known yet, but there are many aspects that are thought to influence it. Along with genetics, these factors are brain structure and chemistry (including the level of serotonin and dopamine in the brain), environmental factors such as socioeconomic factors, and cell-to-cell signaling issues in the brain [1,2,10].
Schizophrenia affects men and women equally and occurs at similar rates in all ethnicities world wide. However, an australian study found that schizophrenia is more common in developed countries and more common in women in developing countries [6]. In fact, schizophrenia ranks among the top ten causes of disability in developed countries worldwide [5]. Roughly 1% of Americans have schizophrenia [2]. Worldwide, roughly 0.7-1.2% of adults have schizophrenia at some point in their lives [3]. Schizophrenia is known to run in families; it occurs in 10% of people with a direct relative, such as a parent or sibling, who have the disease. An identical twin of a schizophrenic has a 40-65% chance of developing schizophrenia [2]. However, schizophrenia is a complex disease, meaning that there are several genes associated with an increased risk for the disease. There is not a single gene that causes schizophrenia [2]. These genes are generally involved in brain development and the formation of important brain chemicals [2]. The exact cause(s) of schizophrenia are not known yet, but there are many aspects that are thought to influence it. Along with genetics, these factors are brain structure and chemistry (including the level of serotonin and dopamine in the brain), environmental factors such as socioeconomic factors, and cell-to-cell signaling issues in the brain [1,2,10].
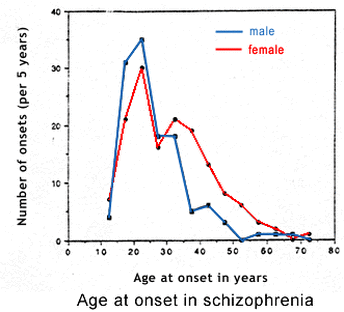
Schizophrenia typically begins in early adulthood, however men tend to develop the disease slightly earlier than women. The disease onset in most men in between 16 and 25 years old, while most women develop symptoms several years later, with the rate of onset in women being noticeably higher in women over 30 years old [5]. The average age of onset is 25 years old in women and 18 years old in men. At the same time, the onset of schizophrenia is rare for individuals under 10 years of age or over 40 years of age [5].
To see a link of famous people that were diagnosed or suspected to have schizophrenia, click here.
To see a link of famous people that were diagnosed or suspected to have schizophrenia, click here.
The Genetics of Schizophrenia: The TOP3B Gene
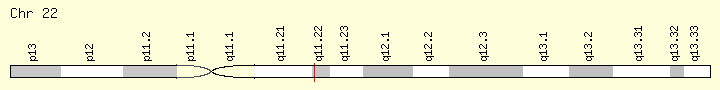
Schizophrenia is a complex disease, and there is no single thing that entirely causes the disease. In July of 2013, researchers published findings that showed a link between a specific human gene and schizophrenia. This gene is the TOP3B gene, with is short for DNA Topoisomerase III Beta. The researchers found a deletion on chromosome 22 that was present at a greater rate than average in Norther Finnish people. This deletion included the whole TOP3B gene and was found at a significantly increased frequency in the schizophrenic individuals than the non-schizophrenic individuals in their sample [10]. Thus, they found evidence suggesting that the gene TOP3B, along with environmental factors, could contribute to the development of schizophrenia in humans [10].
TOP3B encodes for a protein, TOP3β. TOP3β is a DNA topoisomerase, meaning that this protein helps to unwind small segments of the DNA at a time so that other proteins can access it. An example of when this would be necessary is during replication of the DNA [8]. For more detailed descriptions of the gene and the resulting protein, please see the pages entitled 'The TOP3B Gene' and 'The TOP3β Protein'.
Symptoms
The symptoms of schizophrenia include a wide range of cognitive, behavioral, and emotional issues that can be placed into three broad categories: positive symptoms, negative symptoms, and cognitive symptoms [1,2].
Positive symptoms are psychotic behaviors that are not seen in non-schizophrenics. This category includes hallucinations, delusions, thought disorders, and movement disorders. These symptoms may come and go and their severity may change over time [2].
Positive symptoms are psychotic behaviors that are not seen in non-schizophrenics. This category includes hallucinations, delusions, thought disorders, and movement disorders. These symptoms may come and go and their severity may change over time [2].
- Hallucinations: These are scents, physical touches (such as an invisible hand on your shoulder), sounds, and visual images that a person senses when no one else does/they are not actually there. Voices are the most common form of hallucinations in schizophrenics, such as hearing a voice telling you to do something or warning your of something or different voices talking to each other [2].
- Delusions: These are false beliefs that are not based on reality and are not part of one's cultural belief system. For someone with schizophrenia, these delusions are believed to be true even after someone disproves them. Some examples are the belief that the people in the television are sending special messages to them or that their doctor is trying to harm them. The latter is an example of 'delusions of persecution,' which cause one to believe that others are trying to harm them through acts such as harassing, poisoning, cheating, and plotting against them [2]. Delusions can also be associated with paranoia. Paranoid delusions, especially one's relating to doctors or medical practitioners, can lead to individuals refusing medical care, medication, to even go to a clinic or hospital, and to believe that they are even ill at all [3]. Delusions occur in as many as 4 out of 5 schizophrenics [1].
- Thought Disorders: These are unusual or dysfunctional ways of thinking. One form of this is 'disorganized thinking.' This is when a person has organizing and connecting their thoughts. This can also cause disorganized speech. Effective communication can be impaired and when asked questions, their answers may be partially or completely unrelated. It can also lead to inappropriate or out of place laughter [4].Speech may also be garbled, hard to understand, and involve joining meaningless words together. This latter symptom is known as 'word salad' [1]. Another form is 'thought blocking'. This occurs when a person stops speaking in the middle of a sentence; the schizophrenic may say it felt like the thought was taken out of their head. The third form of thought disorders is 'neologisms,' which are meaningless words that a person with a thought disorder makes up [2].
- Movement Disorders: These symptoms may present themselves in a wide range of ways, from agitated body movement to, in the extreme case, as a person becoming catatonic [2]. Often, behavior is unfocused, making it hard to complete tasks. Further examples are repetitive motions, resistance to instructions, inappropriate and bizarre posture, a complete lack of response, and pointless and excessive movement [1]. Catatonia occurs when one does not move nor respond to others. Due to the treatments now available for schizophrenia, catatonia has become rare today [2].
Negative symptoms are associated with disruptions to normal emotions and behaviors. These symptoms can be harder to recognize as being related to schizophrenia and can often be mistaken for depression or laziness, but they are part of the overall disease. These individuals may need help with daily tasks and activities [2]. About 25% of patients with schizophrenia have a condition called the deficit syndrome, defined by severe and persistent negative symptoms [7]. Examples of these symptoms include:
Symptoms in teenagers are similar to those of adults but can be harder to diagnose as schizophrenia as some of the early symptoms can be seen as typical aspects of development during teenage years [1]. Examples are:
- A lack of emotion: not making eye contact, not changing facial expressions, speaking without inflection or in a monotone nature, and not adding hand or head movements to speech [1] (also call the 'flat affect' [2])
- A lack of pleasure or interest in everyday life, social withdrawal or isolation [1,2]
- A lack of ability to plan and carry out activities: decreasing talking, neglect of personal hygiene [1,2]
- Speaking very infrequently, even when forced to interact [1,2]
- Insomnia or oversleeping: having trouble sleeping [4]
- Poor executive functioning: having trouble understanding information and using it to make decisions
- Trouble focusing or paying attention
- Problems with working memory: having trouble using information immediately after learning it [2]
Symptoms in teenagers are similar to those of adults but can be harder to diagnose as schizophrenia as some of the early symptoms can be seen as typical aspects of development during teenage years [1]. Examples are:
- Withdrawal from friends and family or changing friends
- A drop in school performance
- Trouble sleeping
- Irritability or depressed mood
- A lack of motivation
- Compared with adults, teens may be less likely to have delusions and more likely to visual hallucinations [1,2]
Diagnosis
To be diagnoses with schizophrenia, a medical doctor will review the patient's medical and psychological histories, take a physical exam, and conduct medical and psychological exams [1]. Medical exams such as a complete blood count (CBC) and Magnetic Resonance Imaging (MRI) and/or Computed Tomography (CT) scans are used to rule out other conditions with similar symptoms to schizophrenia, such as bipolar disorder, schizoaffective disorder, tumors, and problems with the structure of the brain [1,2]. They must also rule out substance abuse and side affects from medication as being the cause for the symptoms [1]. The physician will also conduct a psychological evaluation, during which they will assess the patient's mental status by observing their appearance and demeanor and asking about thoughts, moods, delusions, hallucinations, substance abuse, and potential for violence or suicide [1].
After ruling out other potential causes, the patient must meet the criteria in the Diagnostic and Statistical Manual of Mental Disorders (DSM) that is published by the American Psychiatric Association. A person must have at least two of the following symptoms most of the time during a one-month period, with some level of disturbance being present over six months:
After ruling out other potential causes, the patient must meet the criteria in the Diagnostic and Statistical Manual of Mental Disorders (DSM) that is published by the American Psychiatric Association. A person must have at least two of the following symptoms most of the time during a one-month period, with some level of disturbance being present over six months:
- Delusions
- Hallucinations
- Disorganized speech
- Extremely disorganized behavior
- Catatonic Behavior, which ranges from a coma-like daze to bizarre, hyperactive behavior
- Negative symptoms
Treatment
While there is no cure for Schizophrenia at the moment, it is now a highly treatable disease. It requires lifelong treatment, even after symptoms have subsided. Treatments are generally guided by a psychiatrist who is experienced in treating this disease. Treatment may also incorporate a social worker, psychologist, psychiatric nurse, and/or case manager to coordinate treatment. The basis and first method of treatment is medication*, mainly antipsychotics, which are thought to control symptoms by affecting the brain neurotransmitters dopamine and serotonin [1]. These medications can take several weeks to show an improvement. Often, the psychiatrist and patient must work together to find the most effective medication and dosage for that particular individual [1]. major determinant in seeing eventual improvements is how consistent and willing the patient is to take their medication(s). If necessary, anti-depressants and anti-anxiety medications can be also added, in conjunction with the antipsychotics, to the patient's treatment plan [1]. Once the proper medication(s) are found, the next important step in treatment are psychological and psychosocial interventions. These may include:
*For a list of side effects of antipsychotic medication, visit the 'treatment' tab here.
- Individual therapy: where an individual can learn to cope with stress and recognize early signs of relapse.
- Social skills training: which focuses on improving communication and social interactions
- Family therapy: which provides support and education to help families cope and live with a relative with schizophrenia
- Vocational Rehabilitation and supported employment: which helps individuals with schizophrenia prepare for, find, and maintain jobs [1]
*For a list of side effects of antipsychotic medication, visit the 'treatment' tab here.
References
[Left Header Image]: From "Pittsburgh Social Security Disability Attorney." Figure 1. Retrieved Feb. 4, 2014 from http://www.pittsburghdisability.com/schizophrenia/
[Right Header Image]: From "Study Explores how Brain Disruption may Foster Schizoprenia." Yale News. Retrieved Feb. 4, 2014 from http://news.yale.edu/2012/09/24/study-explores-how-brain-disruption-may-foster-schizophrenia
[1] Mayo Clinic. (2014). Disease and Conditions: Schizophrenia. Retrieved Feb. 5, 2014 from http://www.mayoclinic.org/diseases-conditions/schizophrenia/basics/definition/con-20021077
[2] National Institute of Mental Health. Mental Health Information: Schizophrenia. Retrieved Feb. 5, 2014 from http://www.nimh.nih.gov/health/topics/schizophrenia/index.shtml?utm_source=publish2&utm_medium=referral&utm_campaign=www.kpbs.org
[3] Nordqvist, C. Medical News Today. (Last updated Oct. 20, 2013). What is Schizophrenia? Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/articles/36942.php
[4] Michael Bengston. Psych Central. (Last reviewed Oct. 9 2013). Schizophrenia and Psychosis. Retrieved Feb. 5, 2014 from http://psychcentral.com/disorders/schizophrenia/
[5] The Internet Mental Health Initiative. (2010). Schizophrenia Facts and Statistics. Retrieved Feb. 5, 2014 from http://www.schizophrenia.com/szfacts.htm#
[6] Medical News Today. (May 31, 2005). Schizophrenia More Common in Developed Nations. Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/releases/25389.php
[7] The Harvard Medical School Family Health Guide. (Last Updated July 2006). The Negative Symptoms of Schizophrenia. Retrieved Feb. 5, 2014 from http://www.health.harvard.edu/fhg/updates/update0706c.shtml
[8] McDowall, J. InterPro. (2014). DNA Topoisomerase. Retrieved Feb. 5, 2014 from http://www.ebi.ac.uk/interpro/potm/2006_1/Page1.htm
[10] Stoll, G., Pietilainen, OP., Linder, B., et. al. Deletion of TOP3β, a component of FMRP-containing mRNPs, contributes to neurodevelopmental disorders. Nat. Neurosci. 2013 Sep;16(9):1228-37. doi: 10.1038/nn.3484. Epub 2013 Aug 4. PubMed PMID: 23912948.
[11] Goodchild, L. Medical News Today. (Mar. 14, 2009). New Brain Study find Schizophrenia Linked to Signaling Problems. Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/releases/141084.php
[Right Header Image]: From "Study Explores how Brain Disruption may Foster Schizoprenia." Yale News. Retrieved Feb. 4, 2014 from http://news.yale.edu/2012/09/24/study-explores-how-brain-disruption-may-foster-schizophrenia
[1] Mayo Clinic. (2014). Disease and Conditions: Schizophrenia. Retrieved Feb. 5, 2014 from http://www.mayoclinic.org/diseases-conditions/schizophrenia/basics/definition/con-20021077
[2] National Institute of Mental Health. Mental Health Information: Schizophrenia. Retrieved Feb. 5, 2014 from http://www.nimh.nih.gov/health/topics/schizophrenia/index.shtml?utm_source=publish2&utm_medium=referral&utm_campaign=www.kpbs.org
[3] Nordqvist, C. Medical News Today. (Last updated Oct. 20, 2013). What is Schizophrenia? Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/articles/36942.php
[4] Michael Bengston. Psych Central. (Last reviewed Oct. 9 2013). Schizophrenia and Psychosis. Retrieved Feb. 5, 2014 from http://psychcentral.com/disorders/schizophrenia/
[5] The Internet Mental Health Initiative. (2010). Schizophrenia Facts and Statistics. Retrieved Feb. 5, 2014 from http://www.schizophrenia.com/szfacts.htm#
[6] Medical News Today. (May 31, 2005). Schizophrenia More Common in Developed Nations. Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/releases/25389.php
[7] The Harvard Medical School Family Health Guide. (Last Updated July 2006). The Negative Symptoms of Schizophrenia. Retrieved Feb. 5, 2014 from http://www.health.harvard.edu/fhg/updates/update0706c.shtml
[8] McDowall, J. InterPro. (2014). DNA Topoisomerase. Retrieved Feb. 5, 2014 from http://www.ebi.ac.uk/interpro/potm/2006_1/Page1.htm
[10] Stoll, G., Pietilainen, OP., Linder, B., et. al. Deletion of TOP3β, a component of FMRP-containing mRNPs, contributes to neurodevelopmental disorders. Nat. Neurosci. 2013 Sep;16(9):1228-37. doi: 10.1038/nn.3484. Epub 2013 Aug 4. PubMed PMID: 23912948.
[11] Goodchild, L. Medical News Today. (Mar. 14, 2009). New Brain Study find Schizophrenia Linked to Signaling Problems. Retrieved Feb. 5, 2014 from http://www.medicalnewstoday.com/releases/141084.php
Kerry Zimdars
Last updated: 1/26/2015
University of Wisconsin-Madison
Last updated: 1/26/2015
University of Wisconsin-Madison